Cicatricial Alopecias (Scarring Alopecia)
Cicatricial Alopecias
Cicatricial alopecias, or “Scarring Alopecias” represent a diverse group of conditions that cause irreversible, scarring hair loss. Cicatricial is the medical term for scarring, and alopecia is the medical term for hair loss. The upper portion of the hair follicle from the bulge area upward is considered permanent, whereas the lower portion is non-permanent. When the scarring process affects the permanent portion, especially near the bulge region and the infundubulum, cicatricial alopecia is more likely. Scarring alopecias in the peri-bulge area can cause irreversible damage and should be considered an emergency to minimize the extent of hair loss.
Broadly speaking, this section will focus on scarring alopecias that are non-infectious in cause even though there may be an infectious component to the process (as will be explained). There are both inflammatory cicatricial alopecias like discoid lupus, lichen planopilaris, and folliculitis decalvans as well as non-inflammatory types like pseudopelade of Brocq and follicular degeneration syndrome. Cicatricial alopecias can also be divided into lymphocytic-mediated (lupus, lichen planopilaris, pseudopelade of Brocq) and neutrophil-mediated (folliculitis decalvans).
Sperling coined the term central centrifugal scarring alopecia (CCSA) that refers to a group of scarring alopecias that are centered principally on the crown/vertex, with progression in a roughly symmetrical pattern. These conditions include pseudopelade of Brocq, follicular degeneration syndrome, and folliculitis decalvans.
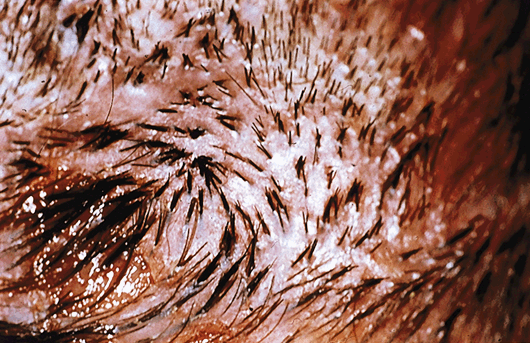
Tufting can occur as an endstage phenomenon in many cicatricial alopecias, as the inflamed infundibulum heals by coalescing with other infundibula. This condition is known as polytrichia.
Lymphocytic-Mediated Cicatricial Alopecias Discoid Lupus
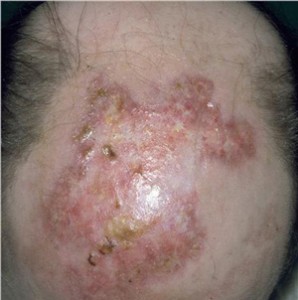 Discoid lupus accounts for 30 to 40% of patients who present with scarring alopecias. Interestingly, less than 10% of patients who present with scalp lupus progress to systemic lupus erythematosus. Patients present with red plaques of hair loss, atrophy, telangiectasias, and follicular hyperkeratosis. Scalp lesions begin as red papules or irregular small scaly plaques. These smaller lesions expand into confluent red and swollen plaques. At this point, the hair loss may still be reversible. The thickened scale that develops may be removed to reveal keratinous plugs that represent follicular hyperkeratosis, which occurs in the center of the plaque that is distinguishable from lichen planopilaris that has the hyperkeratosis toward the periphery. As the lesion expands, the central redness starts to fade and the surface begins to flatten to reveal loss of skin color and atrophy, with the development of scarring. These large, white, flattened placques begin to predominate over the previous red, inflammatory phase.
Discoid lupus accounts for 30 to 40% of patients who present with scarring alopecias. Interestingly, less than 10% of patients who present with scalp lupus progress to systemic lupus erythematosus. Patients present with red plaques of hair loss, atrophy, telangiectasias, and follicular hyperkeratosis. Scalp lesions begin as red papules or irregular small scaly plaques. These smaller lesions expand into confluent red and swollen plaques. At this point, the hair loss may still be reversible. The thickened scale that develops may be removed to reveal keratinous plugs that represent follicular hyperkeratosis, which occurs in the center of the plaque that is distinguishable from lichen planopilaris that has the hyperkeratosis toward the periphery. As the lesion expands, the central redness starts to fade and the surface begins to flatten to reveal loss of skin color and atrophy, with the development of scarring. These large, white, flattened placques begin to predominate over the previous red, inflammatory phase.
Lichen Planopilaris (LPP)
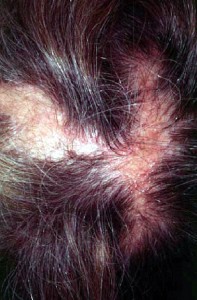 Lichen Planopilaris (LPP) was first described by Pringle in 1895 as lichen planus associated with scalp lesions. LPP accounts for 30 to 40% of scarring alopecias. Usually, LPP occurs between the ages of 30 to 70 with a predominance of females affected (2:1). LPP can be an insidious process with slow development over years with a predilection for areas of high density like the occipital scalp in men with male pattern baldness. Follicular hyperkeratosis occurs along the periphery of the plaques unlike in lupus. Itchiness and tenderness are common features of LPP.
Lichen Planopilaris (LPP) was first described by Pringle in 1895 as lichen planus associated with scalp lesions. LPP accounts for 30 to 40% of scarring alopecias. Usually, LPP occurs between the ages of 30 to 70 with a predominance of females affected (2:1). LPP can be an insidious process with slow development over years with a predilection for areas of high density like the occipital scalp in men with male pattern baldness. Follicular hyperkeratosis occurs along the periphery of the plaques unlike in lupus. Itchiness and tenderness are common features of LPP.
 Pseudopelade of Brocq (PP)
Pseudopelade of Brocq (PP)
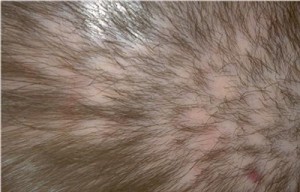
Pseudopelade was first described in 1885 by Brocq in Paris with the term “pelade” meaning alopecia areata in French and obviously, pseudo meaning “like but not really.” Unlike AA which is a non-scarring alopecia, PP is a scarring alopecia with loss of follicular ostia in the affected lesions. Unlike other scarring alopecias, PP is entirely non-inflammatory. Some believe that PP represents a burned-out phase of lupus or LPP but this may not be entirely accurate. PP is a disorder that principally affects adults with patchy hair loss predominantly occurring in the crown and parietal regions that appears like “footprints in the snow”. Although mild redness and itchiness can occur, PP is usually without symptoms and without inflammation. Occasionally, PP may affect the beard area too.
Follicular Degeneration Syndrome (FDS)
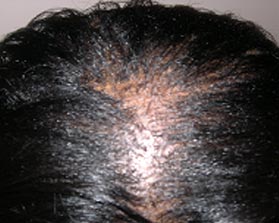 Follicular Degeneration syndrome (FDS) has considerable overlap with PP but today is recognized as a distinct entity. FDS is a non-inflammatory, scarring alopecia that occurs in the crown region and central top of the scalp in African-Americans. Although initially thought to be related to hair-care products, it is now believed to be a disorder without a clear identifiable cause.
Follicular Degeneration syndrome (FDS) has considerable overlap with PP but today is recognized as a distinct entity. FDS is a non-inflammatory, scarring alopecia that occurs in the crown region and central top of the scalp in African-Americans. Although initially thought to be related to hair-care products, it is now believed to be a disorder without a clear identifiable cause.
Treatment of Lupus, LPP, and PP
With less than 10% scalp involvement, topical and injectable steroid should be instituted. Injectable steroid of 2 to 10 mg per ml is injected into the scarred areas once a month and potent topical steroids are applied twice daily. If the patient does not respond well in 8 weeks, hydroxychloroquine is added 200 mg twice daily for a minimum of 6 months. With rapidly progressive alopecia, prednisone dosed at 1 mg per kg per day is given and tapered over 2 months as a bridge therapy until hydroxychloroquine begins to take effect.
With more than 10% scalp involvement, triple therapy is started immediately to include all of the above treatments: topical steroid, injectable steroid, and hydroxychloroquine. Prednisone can also be added in rapidly progressive cases. If no improvement occurs after 6 months, other treatments like isotretinoin, dapsone, and thalidomide may be entertained.
Hair restoration should only be considered with a negative pull test for over 2 years and with stable hair loss. Topical minoxidil has not been clearly established to provide benefit in cases of cicatricial alopecia but has been used as an adjunctive therapy.
Neutrophil-Mediated Cicatrical Alopecias Folliculitis Decalvans (FD)
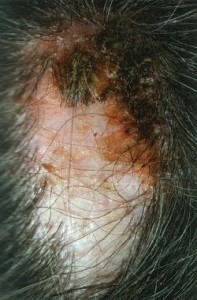 Folliculitis Decalvans (FD) represents a cicatricial alopecia in which there is an abnormal immune response to the normal scalp flora. Tufted folliculitis with embedded hairs exhibiting polytrichia are a common feature in FD. Dissecting cellulitis can present as boggy, inflamed cysts across the scalp.
Folliculitis Decalvans (FD) represents a cicatricial alopecia in which there is an abnormal immune response to the normal scalp flora. Tufted folliculitis with embedded hairs exhibiting polytrichia are a common feature in FD. Dissecting cellulitis can present as boggy, inflamed cysts across the scalp.
Therapeutic treatment involves targeting the staph.aureus infection through combination therapy. Anti-staphylococcal antibiotics such as erythromycin, cephalosporins, trimethoprim/sufamethoxozole, clindamycin, or a fluoroquinalone can be combined with rifampin for added efficacy. Topical and systemic steroids have been used with some success in the treatment of FD. Topical fusidic acid can provide some benefit. For severe dissecting folliculitis, high-dose isotretinoin for a prolonged course may be recommnended. Laser hair removal to remove the offending hair may be necessary for long-term improvements.




