Hirsutism Dallas
Clinical Features of Hirsutism
Hirsutism refers to the excess of terminal hairs in women in anatomic sites that are characteristically considered present in the post-pubescent male. A number of conditions can give rise hirsutism, including disorders involving the adrenal and ovary glands, hyperprolactinemia, hyperinsulinemia, and increased sensitivity to male hormones. Drugs like danazol, Norplant, and anabolic steroids can also have side effects that include hirsutism.
 Polycystic ovary syndrome (PCOS) is by far the most common cause of hirsutism, affecting 6% of women in reproductive age. Stein and Levanthal described this condition involving amenorrhea, obesity, and hirsutism in association with cystic ovaries. PCOS is best characterized as chronic anovulation and hyperandrogenism. Chronic anovulation can present as amenorrhea (no menstruation), oligomenorrhea (menses between 6 weeks to 6 months) or abnormal uterine bleeding. Infertility can be the first sign of anovulation to a woman. Insulin resistance with increased androgen hormones has been found to be a prominent feature in many cases of PCOS but not all. It is thought that hyperinsulinemia may lead to increased ovarian and possibly adrenal androgen production.
Polycystic ovary syndrome (PCOS) is by far the most common cause of hirsutism, affecting 6% of women in reproductive age. Stein and Levanthal described this condition involving amenorrhea, obesity, and hirsutism in association with cystic ovaries. PCOS is best characterized as chronic anovulation and hyperandrogenism. Chronic anovulation can present as amenorrhea (no menstruation), oligomenorrhea (menses between 6 weeks to 6 months) or abnormal uterine bleeding. Infertility can be the first sign of anovulation to a woman. Insulin resistance with increased androgen hormones has been found to be a prominent feature in many cases of PCOS but not all. It is thought that hyperinsulinemia may lead to increased ovarian and possibly adrenal androgen production.
Ovarian androgen-secreting tumors can cause hirsutism. In women with greater than 2.5 times or more of a normal testosterone level should be investigated for such a possible tumor. However, in most cases, simply ovarian hyperplasia without a tumor can account for an elevated testosterone level. An adrenal tumor should be considered with dihydroepiandrosterone sulfate (DHEAS) that is twice the normal value. Similarly, a high prolactin level may indicate a prolatinoma.
Congenital adrenal hyperplasia can account for women with hirsutism with symptoms overlapping those of PCOS. The most common enzyme defect is partial 21-hydroxylase deficiency. Although DHEAS may be elevated with 21-hydroxylase deficiency, 17 alpha-hydroxyprogesterone can be the most specific test for this condition. 17 alpha-hydroxyprogesterone varies with the menstrual cycle and the circadian (daily) rhythm so timing of drawing the assay should be taken during the first 14 days of the menstrual cycle. Cushing’s syndrome can be evaluated by a 24-hour urine free cortisol test.
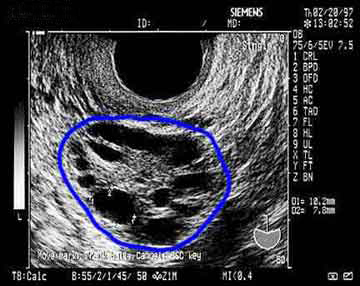
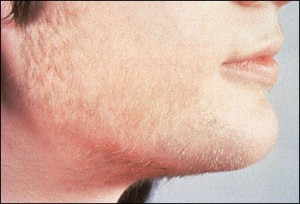
Menopausal women who are not on hormone replacement therapy with estrogen or estrogen plus progestin can show thinning of the axillary and pubic hair due to declining DHEA/DHEAS with increased hirsutism due to the increased ratio of androgen to estrogens. Nevertheless, very high androgen levels should point toward the possibility of a tumor and further evaluation along those lines.
5 to 15% of women who exhibit hirsutism have no definable cause. However, diagnosis of idiopathic hirsutism (unknown hirsutism) must come after appropriate clinical and laboratory evaluations to rule out PCOS and other known causes.
Hirsutism Treatment
Therapy for hirsutism is aimed either at reducing overall androgen production or at the terminal effects of androgen on receptor sites. The first-line therapy is primarily targeted at ovarian suppression with or without supportive treatments. All hormonal therapies require at least 6 to 12 months to exert their benefit.
Ovarian suppression can be undertaken in reproductive-age females using oral contraceptive pills (OCPs). The primary effect of OCPs is to suppress the central nervous system’s gonadotropins (LH and FSH) by which ovulation is blocked. OCPs also cause increased production of SHBG by the liver that serves to decrease free testosterone levels. Also OCPs stimulate the liver ezyme activity to clear existing androgens. In summary, OCPs primarily reduce hirsutism by increasing SHBG and thereby free androgen levels and by decreasing gonadotropin-stimulated ovarian androgen production.
Spironolactone has long been used to treat androgen excess by inhibiting cytochrome P450-related ovarian and adrenal steroidogenesis, 5-alpha reductase, and the androgen receptor. The usual dose of spironolactone is 100 to 200 mg daily depending on clinical assessment. Doses can be reduced after 6 to 12 months of therapy when a response is noted to 75 to 100 mg per day. Side effects of high blood potassium should be kept in mind in those with kidney disease or with excessive dietary ingestion of potassium.
Cyproterone Acetate is a progestagen that can be used to treat hirsutism. Combining OCP 50 micrograms of ethinyl estradiol and 2 mg of cyproterone acetate (Dianette) and 50 mg of cyproterone acetate for prostate cancer are available in Europe and Canada. To treat hirsutism 25 to 100 mg of cyproterone acetate is given daily on days 5 to 15 of the menstrual cycle or with 50 micrograms of ethinyl estradiol on days 5 to 25 or during the first 10 days of the OCP cycle.
Whereas cyproterone acetate is a partial androgen agonist-antagonist, flutamide is a pure anti-androgen that is twice as strong. Dosage for hirsutism is 125 to 250 mg a day. Because of the rare but serious side effect of liver toxicity, flutamide is the least often used anti-androgen.
Five mg dosage of finasteride (Proscar) has been found to be effective in the treatment of hirsutism with the obvious caveat of risk of birth defects in reproductive-age women. The combination of 5 mg of finasteride and 2 mg cyproterone acetate/35 micrograms of ethinyl estradiol (Diane 35) for 2 weeks per month versus Diane 35 alone daily has shown improved effectiveness in hirsutism.





