Telogen Effluvium Dallas
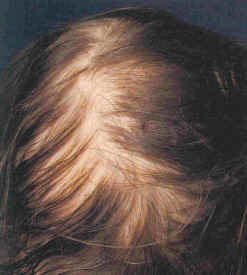
Telogen Effluvium Hair Loss
Telogen effluvium (TE) describes abnormal shedding of telogen hairs so that noticeable shedding and/or hair thinning occurs. Headington proposed 5 mechanisms by which TE can occur. Three mechanisms for telogen effluvium occur in the anagen phase and two occur in the telogen phase:
- Immediate Anagen Release: Follicles that would normally complete a longer cycle of anagen prematurely enter telogen. Typically immediate anagen release has a short time to onset of 3 to 5 weeks from the inciting factor. Drug-induced telogen effluvium may account for this type of TE. See list of drugs that may induce TE at the end of this section.
- Delayed Anagen Release: Hairs are maintained in anagen for longer than usual and then are released into telogen phase at the same time. Postpartum TE is the most common type of this TE in which hairs are kept in anagen during pregnancy then released into telogen after childbirth when there is a rapid TE after delivery.
- Shortened Anagen: If anagen is shortened by 50%, there is a corresponding doubling of telogen hairs. Etitrinate may cause a shortened anagen phase.
- Immediate Telogen Release: Hairs that would normally remain in telogen for the typical 4 to 12 weeks are cycled into anagen within a few days. Minoxidil is an example of a medication that can cause TE by moving the hairs prematurely into anagen phase.
- Delayed Telogen Release: Telogen is prolonged and there is slightly more synchronicity in cycling so that scalp hair falls out at the same time.
Acute Telogen Effluvium
Causes of acute TE include the following: drugs, fever, postpartum, crash dieting, thyroid deficiency, iron deficiency, prolonged anesthesia, malignant disease, renal failure, liver disease, malaborpstion, and psychological conditions.
Drugs
Drugs can cause acute TE, as listed in the tables at the end of this section. Certain classes of medications are known to cause TE like anti-coagulants (heparin and coumadin) with more than 10% of patients experiencing TE in a dose-dependent fashion. Anti-thyroid drugs that induce a state of hypothyroidism may also cause acute TE, like iodine, propylthiouracil, and carbimazole. Psychopharmacologic medications like lithium, valproate, carbamazepine, and tricyclic antidepressants have been implicated in acute TE. Oral contraceptives can cause TE 2 to 3 months after discontinuing treatment, which may be similar to what happens with delayed anagen release in the postpartum setting.
Fever
Fever can cause a severe TE 8 to 10 weeks afterwards. A fever may demand a high metabolic level from the body so that hair growth is impaired. Alternatively or in addition, interferons alpha and gamma that are released during a fever have also been shown to decrease epithelial proliferation that would impair the matrix cells within the follicles.
Postpartum
The state of pregnancy with an increased level of estrogen causes a sustained state of anagen, which is released synchronously into telogen following delivery. During pregnancy, anagen hairs increase from 84% in the first trimester to 94% by the third trimester. Increased hair loss may occur 1 to 4 months following childbirth and may continue for several months. Full recovery is expected in 4 to 12 months. Loss can primarily affect the frontal and temporal hairs and be less severe on subsequent pregnancies.
Crash Dieting
Young women in particular who starve themselves with a low protein diet can induce acute TE. Addition of a small amount of protein to the diet can prevent this problem. Diffuse hair shedding can occur within 1 to 6 months after the onset of a stringent diet. 0 to 1000 kCal per day has been associated with hair loss. Some related problems that may compound or be responsible for TE during a diet are relative decrease in thyroid function and associated increase in the hormone dehydroepiandrosterone during fasting.
Thyroid Influences
Hypothyroidism is a known cause of TE, and diffuse hair loss may be the first and only skin sign of hypothyroidism. A history suggestive of hypothyroidism includes weight gain, cold intolerance, and a low energy level. Thyroxine replacement usually corrects the TE unless the follicles have atrophied from longstanding hypothyroidism. The reverse is also true: very high levels of thyroid hormones can also engender TE.
Iron Deficiency
Iron deficiency with or without anemia has been found in 72% of women with diffuse hair loss. Iron deficiency even in the absence of anemia can cause acute TE. Iron deficiency can also unmask underlying androgenetic alopecia (AGA) in a woman predisposed toward AGA.
Prolonged Anesthesia
Prolonged anesthesia with possible influencing factors of blood loss and surgery can also lead to acute TE with regrowth of hair coming about 4 months afterwards.
Malignant Disease, Kidney Failure, Liver Disease, and Malabsorption
TE may be the first sign of Hodkin’s disease, which is known as “toxic telogen effluvium”. Chronic renal disease may lead to sparse, dry, and brittle hair with even thinning of body hair, including pubic and axillary hair. Liver disease can also cause diffuse hair loss whether the condition is hepatitis, cirrhosis, or fatty liver. Inflammatory bowl disease, particularly Crohn’s disease, has been associated with sparse hair and growth retardation.
Psychological Causes
Although acute anxiety and depression may cause TE, the paucity of literature to support this claim makes this cause relatively uncommon.
Chronic Telogen Effluvium
Diffuse cyclic hair loss in women was first described in 1959 by Guy et al. in otherwise healthy women. A modern term coined by Whiting is chronic telogen effluvium, which is not an uncommon condition. Typically chronic TE affects women between the ages of 30 to 60 years and occurs without a recognizable inciting factor. The degree of shedding can be severe in the early stages with hairs coming out in clumps. Unlike acute TE, chronic TE continues for years in a fluctuating pattern.
Patients are oftentimes concerned that they will progress toward total baldness, but reassurance that they will not progress toward complete baldness is important. Scalp and hair pain can be a related symptom that correlates better with emotional distress than with actual hair loss. In certain cases of chronic TE, women may have low levels of ferritin when using a male reference range even though they may be in the normal female range. Van Neste and Rushton feel that topping ferritin levels off into the male range (over 30 micrograms per liter) may be helpful. Nutritional supplementation is unwarranted, and excessive dietary supplements may actually induce TE.
After ruling out other sources of TE, treatment of chronic TE is focused on two principal methods: topping off ferritin levels and maintaining topical minoxidil 5% twice daily. Patients should of course be warned that minoxidil might cause TE early on when hairs are cycled prematurely from telogen into anagen phase but that this is a temporary phenomenon.
|
Albendazole
|
Fluoxetine
|
Nisoldipine
|
|---|---|---|
|
Aldesleukin
|
Flurbiprofen
|
Nortriptyline
|
|
Altretamine
|
Fluroxamine
|
Octreotide
|
|
Amiloride
|
Foscarnet
|
Olanzapine
|
|
Amiodarone
|
Ganciclovir
|
Omeprazole
|
|
Amitriptyline
|
Grepafloxacin
|
Paroxetine
|
|
Amlodipine
|
Haloperidol
|
Prazosin
|
|
Amoxapine
|
Ibuprofen
|
Propanefenone
|
|
Azathioprine
|
Imapramine
|
Propylthiouracil
|
|
Bromfenac
|
Indomethacin
|
Protriptyline
|
|
Buproprion
|
Ipratropium
|
Risperidone
|
|
Carvedilol
|
Ketoprofen
|
Ropinirole
|
|
Clofibrate
|
Lansoprazole
|
Sertraline
|
|
Clomiphene
|
Levothyroxine
|
Sparfloxacin
|
|
Clomipramine
|
Liothyronine
|
Sulindac
|
|
Desipramine
|
Lisinopril
|
Tacrine
|
|
Diethylstilbestrol
|
Losartan
|
Testosterone
|
|
Diflunisal
|
Meclofenamate
|
Tiagabine
|
|
Dopamine
|
Mefloquine
|
Tizanidine
|
|
Epinephrine
|
Mesalamine
|
Tocainide
|
|
Esmolol
|
Methimazole
|
Trimipramine
|
|
Estramustine
|
Mexiletine
|
Venlafaxine
|
|
Ethionamide
|
Nabumetone
|
Verapamil
|
|
Fenfluramine
|
Naproxen
|
Zaleplon
|
|
Fenoprofen
|
Naratriptan
|
|
|
Flecainide
|
Nefazodone
|
|
Acyclovir
|
Cyclosporin
|
Lamotrigine
|
|---|---|---|
|
Allopurinol
|
Cytarabine
|
Letrozole
|
|
Amantadine
|
Dacarbazine
|
Leuprolide
|
|
Atorvastatin
|
Dactinomycin
|
Loratadine
|
|
Betaxolol
|
Delavirdine
|
Lovastatin
|
|
Bicalutamide
|
Dexfenfluramine
|
Nifedipine
|
|
Buspirone
|
Diclofenac
|
Pentosan
|
|
Captopril
|
Efavirenz
|
Riluzole
|
|
Carbamazepine
|
Fludarabine
|
Rofecoxib
|
|
Celecoxib
|
Gold
|
Tolcapone
|
|
Ceterizine
|
Granisetron
|
Topiramate
|
|
Acitretin
|
Alpha-Interferon
|
Ramipril
|
|---|---|---|
|
Cidofivir
|
Isotretinoin
|
Terbinafine
|
|
Danazol
|
Leflunomide
|
Timolol
|
|
Granulocyte colony
stimulating factor
|
Levobunolol
|
Valproic Acid
|
|
Lithium
|
Warfarin
|
|
|
Heparin
|
Moexipril
|
|
Acebutolol
|
Fluconazole
|
Oral Contraceptives
|
|---|---|---|
|
Acetominophen
|
Fluoxymesterone
|
Oxaprozin
|
|
Acetohexamide
|
Fluvastatin
|
Paramethadione
|
|
Aminophylline
|
Gabapentin
|
Penbutolol
|
|
Aminosalicylate sodium
|
Gemfibrozil
|
Penicillamine
|
|
Amphotericin B
|
Gentamicin
|
Penicillins
|
|
Asparaginase
|
Guanethidine
|
Pergolide
|
|
Astemizole
|
Halothane
|
Pindolol
|
|
Atenolol
|
Hydromorphone
|
Pirbuterol
|
|
Bendroflumethiazide
|
Hydroxychloroquine
|
Piroxicam
|
|
Bisoprolol
|
Indinavir
|
Pravastatin
|
|
Bromocriptine
|
Isoniazid
|
Prazepam
|
|
Carteolol
|
Itraconazole
|
Probenecid
|
|
Carivastatin
|
Ketoconazole
|
Progestins
|
|
Chlorambucil
|
Labetolol
|
Propanolol
|
|
Chloramphenicol
|
Lamivudine
|
Pyrimethamine
|
|
Chlordiazepoxide
|
Levodopa
|
Quazepam
|
|
Chloroquine
|
Loperamide
|
Quinidine
|
|
Chlorothiazide
|
Lorazepam
|
Ranitidine
|
|
Chlorotrianisene
|
Loxapine
|
Ropinirole
|
|
Chloropropamide
|
Maprotiline
|
Saquinavir
|
|
Chlorothalidone
|
Mebendazole
|
Selegiline
|
|
Cimetidine
|
Mephenytoin
|
Simvastatin
|
|
Clonazepam
|
Mesoridazine
|
Sotalol
|
|
Diazoxide
|
Methusuximide
|
Stanozolol
|
|
Dicumarol
|
Methyldopa
|
Sulfasalazine
|
|
Didanosine
|
Methylphenidate
|
Sulfisoxazole
|
|
Diethylstilbestrol
|
Methyltestosterone
|
Thalidomide
|
|
Diflunidal
|
Methysergide
|
Thioguanine
|
|
Dopamine
|
Metoprolol
|
Thioridazine
|
|
Epinephrine
|
Minoxidil
|
Thiothixene
|
|
Esmolol
|
Misoprostol
|
Tiopronin
|
|
Estrogen
|
Mitotane
|
Trazodone
|
|
Ethambutol
|
Mycophenolate
|
Triazolam
|
|
Ethosuximide
|
Nadolol
|
Trimethadione
|
|
Etidronate
|
Nalidixic acid
|
Ursodiol
|
|
Etodolac
|
Neomycin
|
Vitamin A
|
|
Famotidine
|
Nimodipine
|
Zalcitabine
|
|
Felbamate
|
Nitrofurantoin
|
Zidovudine
|
|
Fenofibrate
|
Odansetron
|





