Tinea Capitis Dallas
Tinea Capitis Explained
Tinea capitis is a fungal infection of the scalp and hair that can arise from different genera of dermatophytes, e.g., Microsporum and Trichophyton, depending on the soil, people, and location. Tinea capitis in general is much more prevalent in prepubescent children with spontaneous remissions that can occur at puberty, as surface lipids in the adult skin may serve to inhibit fungal growth. Most adult cases occur in individuals over 60 years of age. However, the exact reason for this fact is not entirely clear.
Microsporum is transmitted from animal to human, whereas T. tonsurans is transmitted from person to person. Presently, T.tonsurans accounts for over 90% of cases in the United States and the United Kingdom. In the U.S., most cases are found in inner city clinics where lower socioeconomic African American children receive care. The thought is that the practice of braiding can expose the stratum corneum to the fungus and the use of hair oils by African Americans can facilitate adherence.
Types of Tinea Capitis
Tinea Capitis can be inflammatory or non inflammatory and present with either focal or diffuse hair loss. The different types of clinical presentations on Tinea Capitis are as follows:
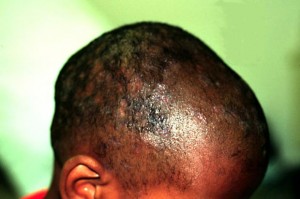
- Diffuse scaling which may be confused with seborrheic dermatitis or psoriasis
- Gray patch accompanied by patchy, scaly hair loss
- black dot with patches of hair loss that represent hairs broken off at the scalp that may resemble alopecia areata.
- Diffuse pustular presentation with hair loss with or without lymphadenopathy
- kerion which is characterized by a boggy mass, usually associated with lymphadenopathy.
There are three recognized patterns of hair invasion: endothrix, ectothrix, and favus. Endothrix and ectothrix account for the majority of the cases. Ectothrix invasions are principally caused by Microsporum in which the cuticle is destroyed, which fragments into masses of spores outside of the hair shaft. The hairs get broken off a few millimeters above the skin surface and appear twisted, brittle and grayish white (gray patch type).
Tinea Capitis Black Dot
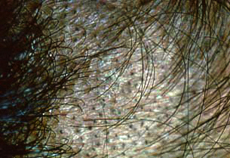
Endothrix infections are caused by fungi that invade and fill the cortex of the hair shaft with masses of spores confined within the cuticle of the hair shaft. The hair shafts are destroyed so that they break off at the scalp surface, which creates the black dot appearance. The most common organism that causes this type of tinea capitis infection is T.tonsurans.
Tinea Capitis Kerion
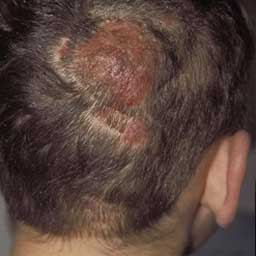 Both M. canis and T. tonsurans can cause a severe inflammatory lesion known as a kerion in a localized area of the scalp. Following 10 days from onset, the area can be severely pustulated with the rapid development of a red plaque to create a raised boggy mass. This represents an immune reaction to the fungus and not a bacterial superinfection. Those with a cell-mediated immunity are the ones that generate a kerion, whereas those who do not have this will most likely not. Despite the degree of swelling, scarring is oftentimes not severe and hair regrowth is expected in most cases.
Both M. canis and T. tonsurans can cause a severe inflammatory lesion known as a kerion in a localized area of the scalp. Following 10 days from onset, the area can be severely pustulated with the rapid development of a red plaque to create a raised boggy mass. This represents an immune reaction to the fungus and not a bacterial superinfection. Those with a cell-mediated immunity are the ones that generate a kerion, whereas those who do not have this will most likely not. Despite the degree of swelling, scarring is oftentimes not severe and hair regrowth is expected in most cases.
Tinea Capitis Ringworm
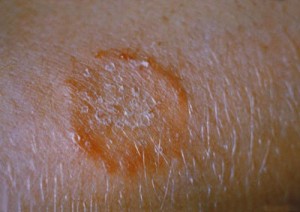
Favus is a type of tinea capitis characterized by scutula, which are sulfuric-yellow concretions of hyphae and skin debris. Favus is caused by T. schoenleinii. Favus, left untreated, can lead to scarring alopecia. Favus is more commonly found in Eurasia and in North Africa but uncommonly in the United States and Western Europe.
Tinea capitis may be suspected when a classic ringworm lesion is found elsewhere on the body. Confirmation of the infection can be undertaken with 20% potassium hydroxide (KOH) preparation. A negative culture is a more accurate indicator of disease eradication than a negative KOH stain.
Oral griseofulvin has been the gold standard of therapy since its introduction in the late 1950s. Newer antifungal medications like itraconazole, fluconazole, and terbinafine have been proposed as more effective given the changing face of causative organisms. When infection is confirmed, all family members must be evaluated with scalp cultures regardless of clinical infection in order to reduce risk of recurrent infection without this measure.
Adjunctive therapies like 2% ketoconazole shampoo, 2.5% selenium sulfide shampoo, 4% povidone-iodine shampoo should be lathered and massaged into the scalp and left on for 5 minutes, which should be repeated 2 to 3 times per week. Preventative measures of similar shampooing regimens should be carried out by close contacts as well. All shared brushes, combs, and bed linens need to be thoroughly disinfected. As kerions are postulated to be an exaggerated local response to the fungus, intralesional steroids have also been proposed so as to prevent scarring and to permit possible faster regrowth of hair.





